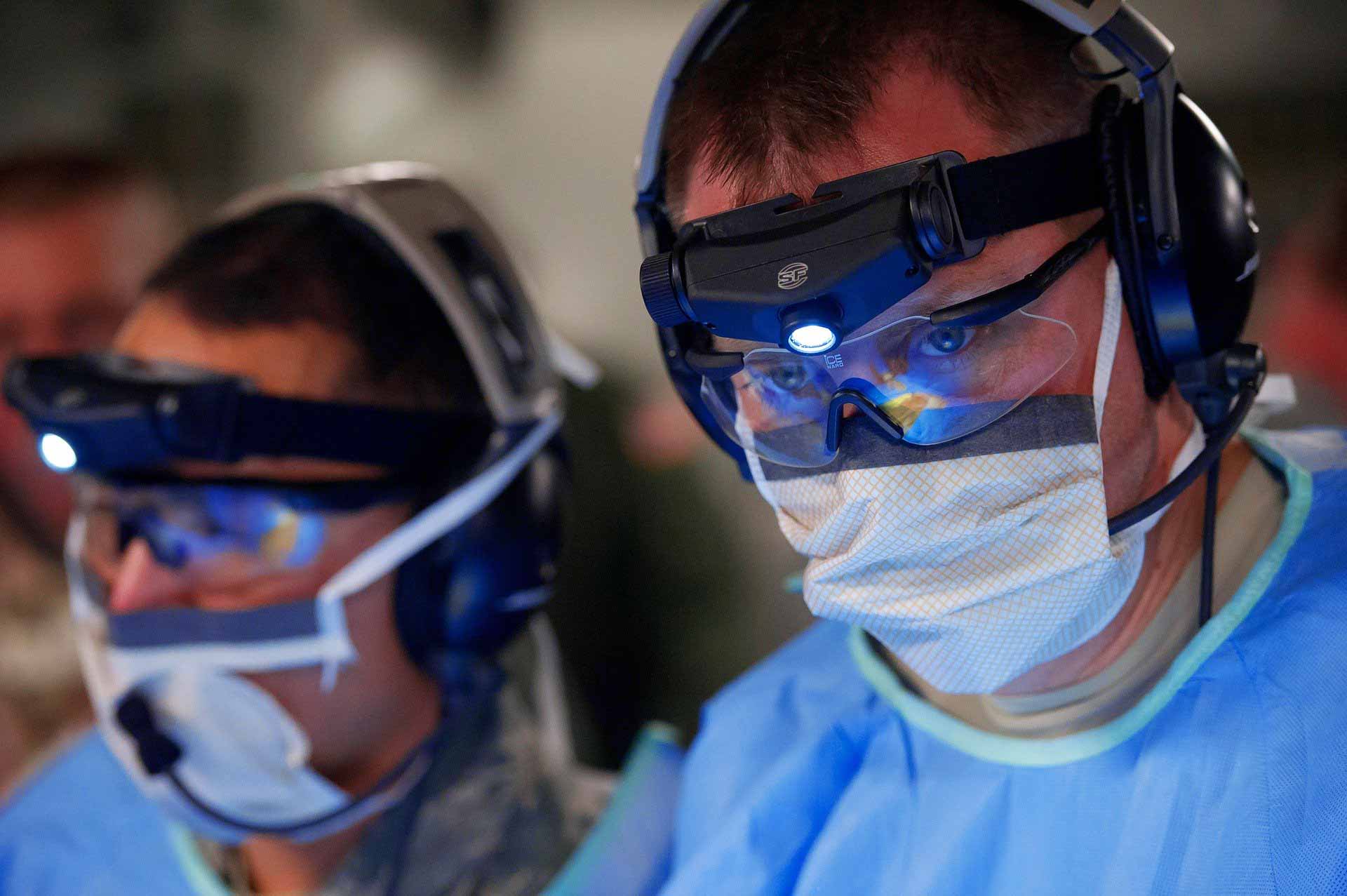
The UN World Health Organization (WHO) highlighted the risks of separating newborns from mothers with a new research. WHO found that up to 125,000 lives could be saved by keeping them together to ensure skin-to-skin contact. In many countries, if COVID-19 infections are confirmed or suspected, newborn babies are being routinely separated from their mothers, putting them at higher risk of death and lifelong health complications, according to the agency.
“Disruptions to essential health services during COVID-19 have severely affected the quality of care provided to some of the most vulnerable babies, and this includes their right to the lifesaving contact they need with their parents”, Anshu Banerjee, WHO Director for Maternal, Newborn, Child and Adolescent Health, said.
According to WHO, the risk is greatest in the poorest countries where the greatest number of preterm births and infant deaths occur, and disruptions to kangaroo mother care – early, prolonged skin-to-skin contact with a parent, and exclusive breastfeeding – will worsen these risks. “Decades of progress in reducing child deaths will be jeopardized unless we act now to protect and improve quality care services for mothers and newborns, and expand coverage of lifesaving interventions like kangaroo mother care”, Dr. Banerjee added. The new research, by WHO and partners, was published in the Lancet EclinicalMedicine.

Kangaroo mother care
WHO said that up to 125,000 babies’ lives could be saved with full coverage of kangaroo mother care. The model of care is particularly important for babies born preterm (before 37 weeks) or at low birthweight (under 2.5 kilogrammes), where it has shown to reduce infant deaths by as much as 40 per cent, hypothermia by more than 70 per cent, and severe infections by 65 per cent. Queen Dube, Director of Health at the Ministry of Health in Malawi, one of the report authors, underscored the benefits.
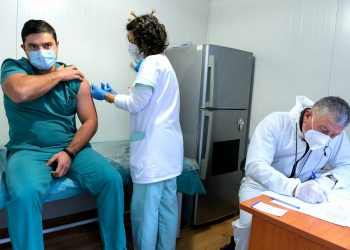
WHO calls to ramp up COVAX production of COVID-19 vaccines
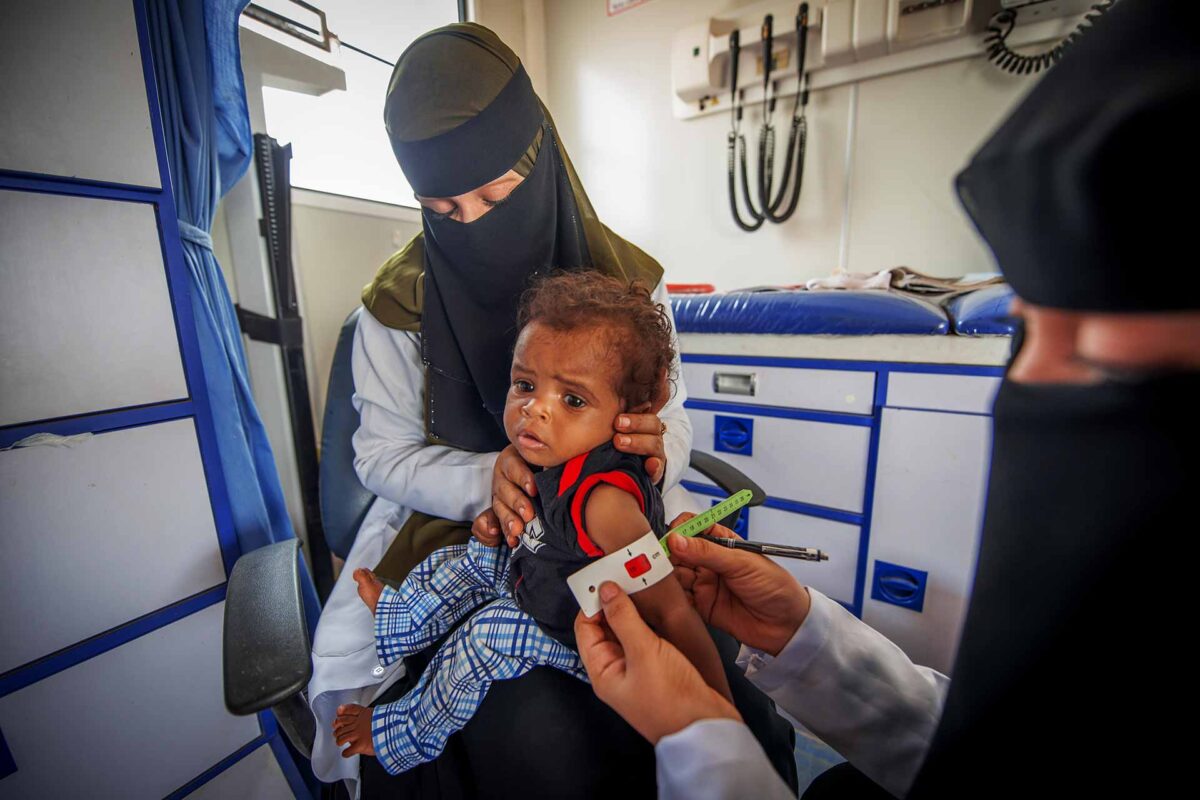
“Kangaroo Mother Care is one of our most cost-effective ways to protect small and sick newborns. According to our analysis, these risks by far outweigh the small chance of a newborn baby getting severe disease from COVID-19”, Dr. Dube said. WHO advised that mothers should continue to share a room with their babies from birth and be able to breastfeed and practice skin-to-skin contact – even when COVID-19 infections are suspected or confirmed – and should be supported to ensure appropriate infection prevention practices.
Low COVID risk
It also noted that studies showed mainly no symptoms or mild disease from COVID-19 in infected newborns, with low risk of neonatal death, with the new study estimating the risk of newborns catching COVID-19 would result in fewer than 2,000 deaths.

However, infection during pregnancy may result in increased risk of preterm birth, which means it is even more important to ensure the right care is given to support preterm babies and their parents during the COVID-19 pandemic, WHO added.
Maternal and newborn health
Maternal health refers to the health of women during pregnancy, childbirth and the postpartum period, whereas perinatal health refers to health from 22 completed weeks of gestation until 7 completed days after birth. Newborn health is the babies’ first month of life. A healthy start during the perinatal period influences infancy, childhood and adulthood.
Maternal, perinatal and newborn health matters to every person, society and country, and should be viewed from both a human rights and wellbeing perspective as highly important topics.
The Sustainable Development Goals (SDGs) are a set of goals set out in 2015 in order to achieve a new sustainable development agenda for the world by 2030. Out of the 17 development goals, number 3 is the goal directly linked to health. Within goal number 3, target 3.1 aims to decrease the global maternal mortality rate to less than 70 per 100 000 live births by 2030.
Postpartum care
Monitoring maternal and newborn health during the postpartum period is critical. The risk of death is highest for newborn babies: 75% of all neonatal deaths occur during the first week of life. Timely detection and management of symptoms have been shown to reduce mortality and complications.
Breastfeeding is optimal for both maternal and child health, and crucial for a healthy start in life. Exclusive breastfeeding for six months provides just the nutrients that newborn babies need and promotes bonding with their mothers. For women, the benefits include a reduced risk of ovarian and breast cancer, and a quicker return to pre-pregnancy weight than with formula feeding.
Women who remain healthy during pregnancy and after birth are more likely to stay healthy later in life. The continuum of newborn, infant, child, adolescent, reproductive, maternal and perinatal health is part of a woman’s life-course. All these stages are interrelated